Cradle cap is commonly found on the heads of babies. But can a 7-year-old get it too? I did some research, and wanted to share what I found. The medical source for this article is from Monica Fisher, M.D, who is a licensed pediatrician.
Can 7-year-olds get cradle cap? Cradle cap is actually a “nickname” for seborrheic dermatitis. It can affect anyone at any age. For reasons of dignity, it is usually called by its true dermatologic title if the person suffering from it is not a baby.
While it is most common in infants, it does appear in older children. The identification and treatment of this mild condition can easily be identified and obtained.
What is Cradle Cap?
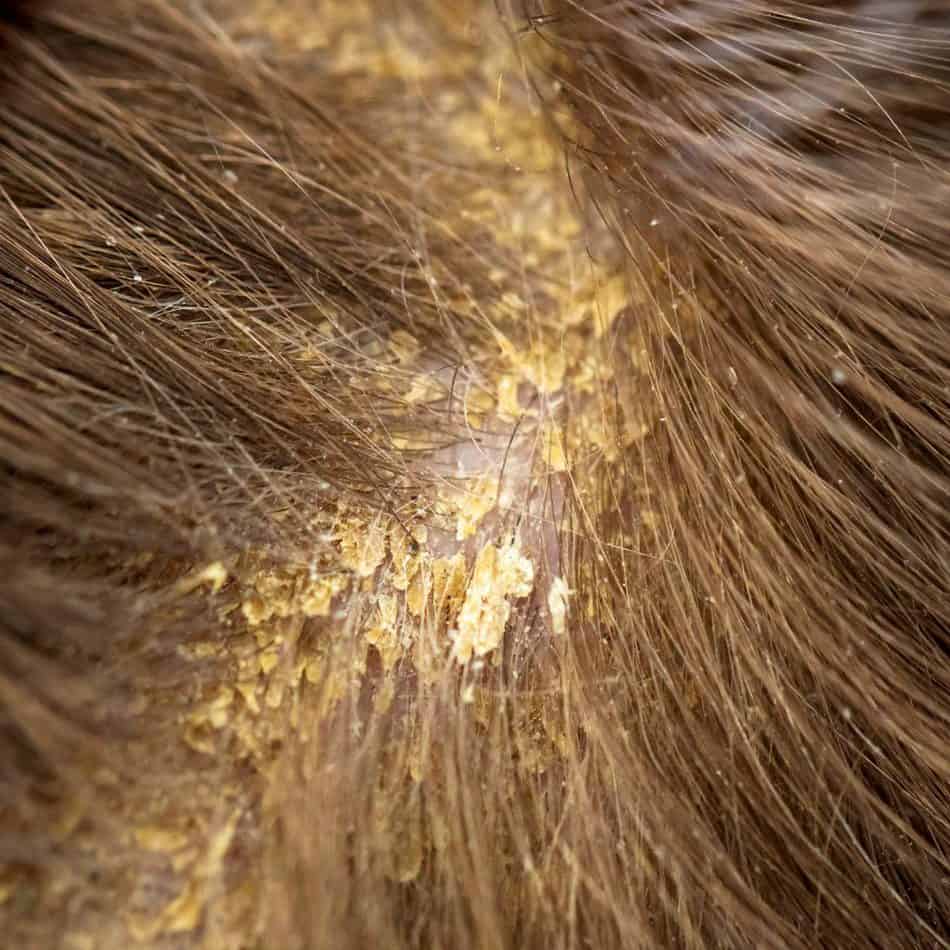
Cradle cap is a yellowish, patchy, greasy, scaly and crusty skin rash that mostly occurs on the scalp of recently born babies. It is usually not itchy and does not bother the baby.
Cradle cap most commonly begins sometime in the first three months but can occur in later years. Similar symptoms in older children are more likely to be dandruff than cradle cap. The rash is often prominent around the ear, the eyebrows or the eyelids. It may appear in other locations as well, where it is called seborrhoeic dermatitis rather than cradle cap.
Some countries use the term pityriasis capitis for cradle cap. It is extremely common, with about half of all babies affected. Most of them have a mild version of the disorder. Severe cradle cap is rare.
In children and adults, the condition is usually referred to as seborrhoeic dermatitis instead of cradle cap, usually to preserve the dignity of those who suffer from it that are not, in fact, sleeping in a cradle.
What Causes Cradle Cap?
Cradle cap is not caused by bacterial infection, allergy or poor hygiene. Cradle cap is also not contagious. Doctors do not agree on what causes cradle cap, but the two most common hypotheses are fungal infection and overactive sebaceous glands. Cradle cap is an inflammatory condition.[
A common cause of cradle cap appears to be a common manifestation of biotin insufficiency. This may be due, in part, to the influence of biotin on fatty acid biosynthesis. Possibly it has to do with overactive sebaceous glands in the skin of newborn babies, due to the mother’s hormones still in the baby’s circulation. The glands release a greasy substance that makes old skin cells attach to the scalp instead of falling off as they dry. There may be a relationship with skin yeasts (Pityrosporum ovale, newly renamed Malassezia furfur).
When to be Worried
If the condition thickens, turns red and irritated, starts spreading, appears on other body parts, or if the child develops thrush (fungal mouth infection), or fungal ear infection (an ear infection that does not respond to antibiotics), medical intervention is recommended.
Severe cases of cradle cap, especially with cracked or bleeding skin, can provide a place for bacteria to grow. If the cradle cap is caused by a fungal infection which has worsened significantly over days or weeks to allow bacterial growth (impetigo, most commonly), a combination treatment of antibiotics and antifungals may be necessary.
Since it is difficult for a layperson to distinguish the difference between sebaceous gland cradle cap, fungal cradle cap, or either of these combined with a bacterial infection, medical advice should be sought if the condition appears to worsen.
Cradle cap is occasionally linked to immune disorders. If the child appears ill and has other problems (e.g. diarrhea), a doctor should be consulted.
Treatment
To help with cradle cap, parents can gently massage their child’s scalp with their fingers or a soft brush to loosen the scales. They may want to shampoo the child’s hair more frequently (no more than once a day), and after shampooing gently brush the scalp with a soft brush or a terrycloth towel.
Oil remedies can be used by rubbing a small amount of pure, plant-derived oil (coconut oil, pure olive oil, almond oil) on the child’s scalp and leaving it on for 15 minutes. After 15 minutes, gently comb out the flakes with a fine tooth comb or brush. Be sure to wash out all of the oil to avoid making the cradle cap worse.
In cases that are related to fungal infection, such as Tinea capitis, doctors may recommend a treatment application of clotrimazole (commonly prescribed for jock itch or athlete’s foot) or miconazole (commonly prescribed for vaginal candidiasis).
Doctors may recommend a treatment with a mild dandruff shampoo such as Selsun Blue even though the treatment may cause initial additional scalp irritation. A doctor may instead prescribe an antifungal soap such as ketoconazole (2%) shampoo, which can work in a single treatment and shows significantly less irritation than over-the-counter shampoos such as selenium disulfide shampoos.
Scalp, Ears, and Eyebrows
If the cradle cap is not severe, it could simply be combed out gently after bathing. The softened scales can then be brushed away with a soft brush, comb or cloth, but if not done very gently, this could worsen the condition and bring about temporary hair loss. Applying petroleum jelly (e.g., Vaseline) liberally overnight is another popular treatment. The softened scales either fall off during the night, or can be brushed off in the morning.[c
There is broad disagreement regarding the role of shampoos. Some sources warn against frequent shampooing, others recommend it. Mild baby shampoo is often recommended, but the exact denotation of the label “mild” in this context is not quite clear. Baby shampoos often contain detergent surfactants, perfumes, quaternium-15 and other eczemagenic irritants. No studies have been performed on non-prescription shampoos.[v
In stubborn cases some doctors may recommend keratolytic (dandruff) shampoos (e.g. with sulfur, selenium, zinc pyrithione, or salicylic acid) while others warn against the use of medicated shampoos in newborns due to systemic absorption. Dandruff shampoos often contain sodium dodecyl sulfate, a noted skin irritant.[
Steroid and tar preparations have also been used but may have drawbacks.
Ketoconazole shampoos and creams are currently shown to be the most effective medical treatment of moderate to serious cradle cap. Research indicates that this anti-fungal medication is not absorbed into the bloodstream.
Eyelids
Typical medical advice is to use baby shampoo, diluted with warm water, on a cotton swab to cleanse the eyelid. There is no agreement on the dilution, which ranges from as high as a 1:1 mix to as low as a few drops of shampoo per half-cup of water.
Related Questions
How can I tell the difference between cradle cap and dandruff? It is possible that your 7-year-old may be suffering from dandruff instead of cradle cap. The difference is that dandruff causes large, oily flakes that are yellow or white, and may come with oily, red, scaly skin. Cradle cap manifests in smaller, dry flakes and comes with dry skin on other parts of the body.
Do I need to shave my child’s head if they have cradle cap? Shaving your child’s head will do nothing to help the cradle cap. Don’t do this. The only thing that shaving the head will accomplish is to bring an exceedingly large amount of embarrassment to the child. Instead, try the treatments listed above, such as shampoo, and gentle combing after each bath or shower. Vaseline and mineral oils may also help.
Do I need to treat cradle cap to get it to go away? Usually, cradle cap will go away on its own, with time. However, if your 7-year-old is experiencing distress due to the condition, you may try to treat it with shampoos, combing, or petroleum jelly to expedite the curing process. If you suspect that your child may be suffering from an infection, contact your pediatrician and schedule an appointment to meet and discuss with him or her.